eBusiness Weekly

Mr M. C Wazara Specialist General Surgeon
The skin of a human being is the largest organ in the body. It has many complex functions, such as to keep body parts and fluids in and to create a protective barrier preventing outside germs from entering the body. It helps to regulate the body temperature by changing the amount of blood that flows through the skin.
The skin protects from harmful effects of the sun and other elements. The skin is also a symbol of beauty and giver of confidence to an individual.
In average, man’s skin, if spread out would cover an area of 2m2, (about the same area as a 10-seater dining room table) and it is divided into three main layers:
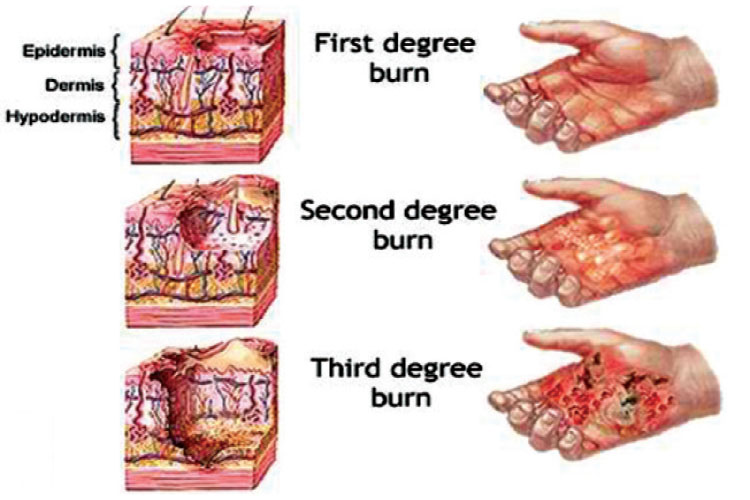
- The outer layer (Epidermis).
- The middle layer (Dermis) which supports the epidermis and has the roots of hair, sweat glands and skin oil glands.
- The deep layer which has the fat, muscles and other deeper organs.
In a burn injury, if only the epidermis is involved, this is considered a superficial or first degree burn.
If the dermis is involved, then we have a partial thickness or second degree burn. Any burn deeper than that is considered a third degree burn or full thickness burn.
Burn injuries are on the rise in Zimbabwe and are a major cause of death, disability, pain, disfigurement and expense to victims.
Who is at risk of being burnt
- Children especially under the age of three years, because of their curiosity, hyperactivity and inability to get away from heat fast enough.
- The elderly and disabled, also because of inability to get away quickly.
- Workmen in high risk environments (factories, agricultural establishments).
- Road traffic victims.
- Epileptic patients, because the flickering of fire can trigger fits. Once fits start the victim becomes unconscious and is unable to move away from the fire.
- People with depression and mental illness — people still attempt to commit suicide by burning themselves.
- Victims of criminal attacks —acid splashes to the face are common malicious attacks abroad and locally by individuals intending to disfigure their victim.
- Altered mental status — people on sleeping medication, intoxicated with alcohol or drunk on recreational drugs are at greater risk of receiving burns.
Anyone else of course can suffer burn injury, but the above categories are at greatest risk.
Effects of burns
The burn injury destroys the skin to varying degrees of depths, but causes the following in all patients:
Pain: This can be so severe, that only the strongest painkillers can control the pain. This is because nerves that are usually covered by skin are now exposed. (Imagine ten or twelve tooth aches all at once).
Malnutrition: Once burnt the body needs extra ordinary amounts of calories and protein to be able to heal itself. This requirement can be as much as four times the usual requirements and victims failing to get adequate nutrition may fail to recover.
Loss of body fluids: Once skin cover is lost, patients lose fluids through the open wound, which is the main cause of death and kidney failure in the first few days. The fluid losses must be replaced and usually in hospital.
Loss of temperature control: Patients who lose significant amount of skin are at risk of developing HYPOTHERMIA (low body temperature), which is extremely hazardous and can be often fatal, especially in children. They must be nursed in a warm environment.
Infection: Most deaths in burns after the first week are due to infections. With the protective barrier gone, bacteria enters the body and bloodstream and can end the life of the patient. Large burns must be managed by those qualified to do so and preferably in a facility designed to look after burns.
Agents that cause burns
Sun and Radiation: especially in pale skinned people and in people exposed for long periods.
Hot water and liquids: probably the most common, also known as scalds.
Electricity: one of the most dangerous because high voltage injuries are internal and not obvious initially. It damages the kidneys often and can destabilise the heart.
Fire. Friction of the skin in road accidents or sports.
Cold: can damage layers of the skin in the same way as hot agents.
Chemicals: such as acids, alkalis and solvents.
Once a person is burnt, the percentage burnt is the initial major concern. In Zimbabwe, patients with 40 percent area burnt are unlikely to survive.
Patients with the following injuries should always be admitted:
More that 10 percent skin loss in a child.
More than 15 percent skin loss in an adult.
All electric and chemical burns.
All burns where smoke has been inhaled.
All burns of the face, hands, feet, private parts and over joints.
Here is how to prevent
- Keep children out of the kitchen.
- Turn handles of pots towards the back of the stove.
- If bathing in a dish, put cold water first, then add warm water to build up the desired temperature. (Most kids burnt by bath water jump into the dish with hot water while the adult is getting the cold water).
- Have fire extinguishers at home.
- Cover all electrical outlets.
- Keep chemicals out of reach.
- Smoke outside — better still don’t smoke.
- Learn First Aid.
Some information
Bathwater should be 1o to 2o above body temperature (40o-43o is maximal).
Third degree burns can occur very easily with hot liquid:
At 65oC you need 2 seconds to make 3o burn.
At 60oC you need 6 seconds to make 3o burn.
At 54oC you need 30 seconds to make 3o burn.
NB: Tea and coffee are usually served at 71oC
What to do when a burn is happening
- Stop the burning safely:
Remove patient from heat source.
Put out the fire.
If ablaze, “stop, drop, roll”. Stop running, it fans the flame. Drop to the ground and roll to extinguish flames.
Switch off electrical source safely or remove patient with non-conducting device.
- Cool the burn:
Copious amounts (20minutes) of room temperature water for burns. No urine, eggs, paraffin or margarine
- Remove clothing.
- Protect burn with clean cloths
- Transfer to a centre that can care for burns.



